Griffith University medical students are getting their first taste of telehealth as they diagnose and treat simulated patients via webcam.
While telehealth emerged as a way to avoid the doctor’s office during a pandemic, it is set to stay, transforming the way many access healthcare.
More than 200 Medical and Pharmacy students have fulfilled their Interprofessional Learning (IPL) and Clinical Communication Skills practice by using online meeting program Microsoft Teams, with 18 simulated patients role-playing six different 10-minute scenarios.
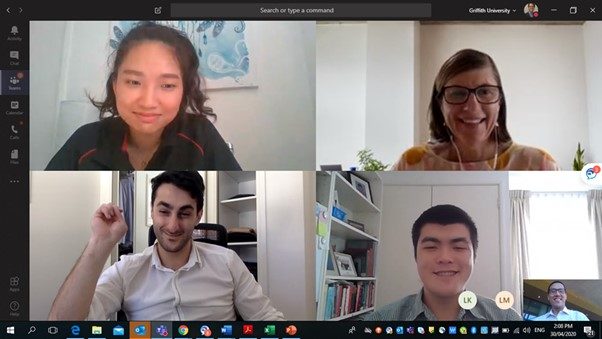
Students get a taste of telehealth.
“Telehealth allows patients who have the IT support to access medical care much easier,” School of Medicine Senior Lecturer Dr Kwong Chan said.
“It is definitely a big part of the future of health care when the technology is able to link all the data together and allow consultation to be done electronically.
“Face-to-face communication skills IPL workshops were converted to online delivery and a positive outcome is that it equips educators for online teaching and prepares students for telehealth.”
Fifteen facilitators guide small groups of six students through 2.5 hour workshops where students interact with simulated patients as they join an online discussion.
Facilitators practicing telehealth.
“Each student had a medical history-taking task to complete,” Dr Chan said.
“The group members — including the simulated patient – observed the interaction, had 10 minutes for reflection and provided constructive feedback.”
Medicine student Holly Miller said the shift from in person workshops to online had provided unexpected benefits.
“Although stemming from unfortunate circumstances, the use of this time to provide training in telehealth has certainly been a positive outcome of learning from afar,” Holly said.
“The session gave students, like myself, a real life practice at performing a telehealth appointment, with all the intricacies that come with technological faults, and learning how to breach the communication barriers that exist online.”
Dr Chan agreed that both students and facilitators had benefited from the online workshops.
“(Moving online) helps to equip educators for online teaching and prepare students for telehealth,” Dr Chan said.
“It allows the students to appreciate the difficulties and challenges of online consultation, but it also encourages students to be flexible and creative.”
Dr Chan also said another unintentional outcome of the workshop was the social connection and support it provided during isolation.
“The lockdown left many of our students feeling isolated and they overwhelmingly appreciated the online interaction with their peers and facilitators,” Dr Chan said.
“Our previous face-to-face workshops focused on affective learning and personal reflection, while the online learning experience offered an opportunity for students to debrief the impact of the pandemic and gain support from each other.”
He said the new way of learning could continue as telehealth ingrains itself as an everyday health service.
“COVID-19 will definitely create a new group of consumers who prefer telehealth.
“We are keen to conduct similar sessions online in the coming year to continue to prepare students for telehealth.”
